Laguna Hills, CA 92653
Shingles
Doctor’s View:
Shingles
Nili N. Alai, MD, FAAD and DENA THOMPSON, B.S., M.S.
Shingles, or herpes zoster, is a very common painful, blistering viral rash that is caused by reactivation of the chicken pox
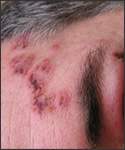
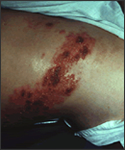
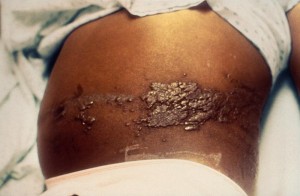
virus called Varicella Zoster Virus (VZV). Shingles occurs in people who have previously been infected with or vaccinated against the chicken pox virus at some point in their lives. Shingles usually occurs as a unilateral pain, burning, or tingling and blistering rash extending in a line pattern from the spinal nerves or facial nerve roots. Common shingles areas include the face, abdomen, back, buttocks, and chest. Red patches form in a belt-like pattern across these areas, and then become small blisters that may be similar in appearance to chicken pox. The rash which clears on its own within two to three weeks, begins to clear after the blisters break and dry into scabs.
Once people have had a single bout of chicken pox, the virus lies dormant in the spinal cord or facial nerve roots. It is thought that when a person has an overall weakened immune system or when their immunity to the varicella virus begins to wane, the virus can reactivate and presents as shingles. Although shingles may happen at any age, it is most common in the 5th-6th decades of life. Typically, shingles usually occurs most commonly in older adults over the age of 60 or those who are immunosuppressed like in HIV, AIDS, or cancer.
Most people only get shingles once in their life. While it is not impossible to get shingles more than once, a recurrence would as probable as getting struck by lightning twice.
Shingles is often a severely painful skin condition. Some people may have pain in the general area days to weeks before the onset of the blisters. The most important clue to shingles diagnosis is unilateral pain and blisters on the skin. A typical shingles eruption never crosses the midline of the body and occurs only on one side: right or left. Extremely rare cases of shingles may become diffuse and spread to the entire body in patients with a very compromised immune system like rheumatoid arthritis patients on multiple drugs including prednisone and methotrexate.
Common symptoms experienced with shingles include flu-like symptoms like chills, fever, and fatigue, along with abdominal and back pain when those skin dermatomes are involved. In some cases, when the virus has affected the facial area, people can experience loss of eye motion, drooping eyelids, taste problems, facial pain, headache, and hearing loss.
Effective treatments are available to help lessen the impact of shingles. For best prognosis and fastest recovery, early start of oral antiviral pills is most important. All shingles cases will eventually resolve with or without treatment.
Treatment started at the earliest stage of symptoms is helpful in shortening the duration and severity of the symptoms. Oral antihistamines like Benadryl may be used for itching, as well as oatmeal baths and calamine lotion. Analgesic medications like ibuprofen (Advil or Motrin), Tylenol, or Vicodin can be used for severe pain.
The most difficult complication of shingles tends to be the residual pain that may last in the area for months or years. Chronic pain lasting more than six weeks after the onset of shingles is called post-herpetic neuralgia (PHN). Antiviral medications including acyclovir (Zovirax) if given within the first 48-72 hours of the occurrence of symptoms, can help reduce the length and severity of post-herpetic neuralgia. Additional treatments are available for PHN.
Shingles is generally not contagious to those who have had chicken pox. Rarely, it may cause problems in pregnant women, infants, immunocompromised individuals, or people who have never had chicken pox. Touching the blisters or blister fluid may cause transmission of the varicella virus.
Varicella Zoster virus is not “curable” because the virus stays dormant in the body for life. Once someone is initially exposed to the varicella virus, an immunity develops which generally prevents a second bout of typical chicken pox. However, this immunity may fade over time making older adults more prone to a later onset of a limited recurrence of the chicken pox virus as shingles.
Testing for shingles may include viral cultures, Tzanck prep ( microscopic exam and staining of skin), and blood testing for titers of antibidies to the varicella virus.
Shingles prevention steps include vaccination( see below). There is a U.S. FDA approved vaccine (Zostavax) for adults age 60 and greater to help lessen the risk of shingles. Zostavax is a live attenuated vaccine and therefore carries a small risk of shingles when administered. There is also an U.S. FDA approved chicken pox vaccine called Varivax used primarily in single dose for children between 12 and 18 months of age, or older who have not had chicken pox.
Shingles
- Shingles typically begins as painful, burning, or tingling sensations with blister formation
- Shingles occurs in people who have had chicken pox or been vaccinated against, and usually in adults over the age of sixty.
- In shingles, blisters erupt and slowly dry out over 2-3 weeks.
- Shingles is not contagious once the blisters have dried.
- Shingles clears spontaneously even without treatment.
- The most difficult complication of shingles is severe, chronic pain called post-herpetic neuralgia.
- Oral antiviral medications can be given to reduce the length and severity of shingles and lessen the risk of post-herpetic neuralgia.
- Treatment is most effective if shingles is diagnosed within the first 48 to 72 hours of symptoms.
General Questions about the Shingles Vaccine
Is there a vaccine to prevent shingles?
Yes. CDC recommends Zostavax for use in people 60 years old and older to prevent shingles. This is a one-time vaccination. Zostavax does not treat shingles or post-herpetic neuralgia (pain after the rash is gone) once it develops.
Is the shingles vaccine safe?
The FDA has licensed the vaccine as safe. The vaccine has been tested in about 20,000 people aged 60 years old and older. The most common side effects in people who got the vaccine were redness, soreness, swelling or itching at the shot site, and headache. CDC, working with the FDA, will continue to monitor the safety of the vaccine after it is in general use.
The shingles vaccine is made of a weakened form of the chickenpox virus. Can a person who has received the vaccine infect others with this virus? Updated Oct 2008
No. It is safe to be around infants and young children, pregnant women, or people with weakened immune systems after you get the shingles vaccine. Transmission of the chickenpox virus from a person who has received the shingles vaccine has never been documented. (For more information on transmission of shingles, read the Shingles Disease Q&A.)
Some people who get the shingles vaccine will develop a chickenpox-like rash near the place where they were vaccinated. As a precaution, this rash should be covered until it disappears.
How effective is the shingles vaccine? Updated May 2009
In a clinical trial involving thousands of adults 60 years old or older, Zostavax reduced the risk of shingles by about half (51%) and the risk of post-herpetic neuralgia by 67%. While the vaccine was most effective in people 60-69 years old it also provided some protection for older groups.
How long does the shingles vaccine last? New May 2009
Research suggests that the shingles vaccine is effective for at least six years, but may last much longer. Ongoing studies are being conducted to determine exactly how long the vaccine protects against shingles.
Who should NOT get the shingles vaccine? NEW May 2009
Some people should not get the shingles vaccine:
- People who have had a life-threatening allergic reaction to gelatin or the antibiotic neomycin.
- People who have a severe allergy to any component of the vaccine.
- People with a weakened immune system as a result of leukemia, lymphoma, or any other blood or bone cancer.
- People with HIV/AIDS who have T-cell counts below 200.
- People being treated with drugs that affect the immune system, including high-dose steroids.
- Women who are or might be pregnant.
Can the shingles vaccine be given to people who have already had shingles?
Yes. People who have had shingles can receive the shingles vaccine to help prevent future occurrences of the disease. This is true no matter when they first got shingles. Updated Oct 2008
How long must a person wait after having shingles to receive the shingles vaccine? Updated Oct 2008
There is no specific time that a person must wait before receiving the shingles vaccine. The decision on when to get vaccinated should be made with your doctor and be based on your specific circumstances. Generally, a person should make sure that his or her shingles rash has disappeared before getting vaccinated.
Why is the shingles vaccine only recommended for people 60 years and older?
A person’s risk for getting shingles begins to rise around age 50. However, shingles vaccine (Zostavax) is only recommended for persons age 60 and older because the safety and effects of the vaccine were only studied in this group, which accounts for about half of all cases of shingles occurring each year in the United States. Future research will determine if the recommended age for vaccination should be lowered.
Shingles occurs in people who have already had chickenpox. Does it matter if a person remembers having had chickenpox? Updated Oct 2008
Anyone 60 years of age or older should get the shingles vaccine, regardless of whether they recall having had chickenpox or not. Studies show that more than 99% of Americans ages 40 and older have had chickenpox, even if they don’t remember getting the disease.
Is it ‘worth it’ for older people to get the vaccine? Updated May 2009
Yes. The older a person is, the more severe the effects of shingles typically are, so all adults 60 years old or older should get the shingles vaccine. There is no maximum age for getting the shingles vaccine.
Does the shingles vaccine, which protects against herpes zoster, also protect against genital herpes? Updated Oct 2008
No. The shingles vaccine is specifically designed to protect people against herpes zoster, which is another name for shingles disease. It will not protect people against other forms of herpes, such as genital herpes.
Is the shingles vaccine covered by insurance? Updated May 2009
All Medicare Part D plans cover the shingles vaccine. The amount of cost-sharing (money you have to pay) for vaccination varies.
Medicare Part B does not cover the shingles vaccine. If you have private insurance or Medicaid, your plan may or may not cover the vaccine; contact your insurer to find out.
For more information, please call (949) 582-7699 or visit the practice website at www.lagunaskincenter.com.
Vaccines and Preventable Diseases:
Shingles (Herpes Zoster) Vaccination
Shingles is a painful localized skin rash often with blisters that is caused by the varicella zoster virus (VZV), the same virus that causes chickenpox. Anyone who has had chickenpox can develop shingles because VZV remains in the nerve cells of the body after the chickenpox infection clears and VZV can reappear years later causing shingles. Shingles most commonly occurs in people 50 years old or older, people who have medical conditions that keep the immune system from working properly, or people who receive immunosuppressive drugs.
Shingles vaccine was recently recommended by the Advisory Committee on Immunization Practices (ACIP) to reduce the risk of shingles and its associated pain in people 60 years old or older.
FOR SHINGLES PAIN:
What is TENS ? How does it work?
A relatively new modality is a transcutaneous electrical nerve stimulation device, hereafter referred to as TENS.
TENS is a low-voltage electrical impulse generator used as a non-pharmacological pain control
device. It usually looks like a portable transistor radio and can be attached to one
belt. Properly turned on, patients are able to use this device as they go about their daily activities.
This special unit has 2-4 electrodes with removable gel based safety pads.
The electrodes are placed on the patient body at positions selected based on your area of pain or itching. Sometimes moving around the pads may help pinpoint special areas based on on various factors such as the anatomical location of peripheral nerves and/or the ara of gratest pain.
Most Notalgia Paresthetica patients find the ideal placement is as the back of the neck at the base where it joins the upper back. Moest people carry most of their tentsion in their neck and upper shoulders. TENS is most effective in reducing the itching in notalgia (mostly the middle of the back) by having treatment on the neck around levels C4-C7.
However, an element of trial and error is always present when determning individual placement. After the electrodes placed with conducting jelly between them and the patient’s skin, the controls are set, the unit
is turned on, and a pulsating current passes through the area providing a mild-to-moderate
stimulation. Some practitioners prefer low frquency/high intensity stimulation while others
favor high frequency/low intensity application. The literature and clinicians both report variations
in treatment time, ranging from 15 or 20 minutes daily to use throughout the day. They
also stress the importance of evaluating your progress and checkin in with your doctor regularly.
Exactly how relief is achieved is not fully known, but there are two prevalent theories: one,
the Gate’ Control Theory, suggests that the pulsating current overloads the nerve circuit and
blocks pain signals to the brain; another theory says that electrcal stimulation causes the brain
to react by releasing natural pain-suppressing substances called enkephelins and endorphins.
A literature review indicates that TENS does not cure a disease and does not work in all cases,
but may give symptomatic relief of pain. Most clinicians agree that TENS applied properly
can be effective. Although some clinicians report as much as a 90 percent success rate with TENS in
carefully selected patients, most report about a 40-50 percent success rate.
As with any medical condition, no two individuals are alike and therefore repsonses vary. TENS may not work equally as well for everyone with Shingles pain.
- On or near the eyes
- In the mouth
- Transcerebrally (on each temple)
- On the front of the neck (due to the risk of acute hypotension through a vasovagal reflex)
- On areas of numb skin/decreased sensation
- On broken skin areas or wounds
- On or near the trigeminal nerve ( face) if you have a history of herpes zoster induced trigeminal neuralgia (Postherpetic neuralgia)
Do not turn TENS up too high as this can cause over-stimulation which may make pain worse. There should be no muscle contraction. TENS should also be used with caution in people with epilepsy or pregnant women (do not use over area of the uterus as the effects of electrical stimulation over the developing fetus are not known). TENS should not be used by people with an artificial cardiac pacemaker due to risk of interference and failure of their implanted device. Possible failure of these warnings can result in a cardiac arrhythmia. In the situation where low frequency (or acupuncture-like) TENS is being used, it is necessary to increase the intensity of the stimulation to the point where a demonstrable muscle twitch is evident. This 2-6Hz (pulses per second) output increases the systemic release of endorphins which in turn cause pain relief.
Information in this publication and site is not intended to serve as medical advice. Individuals may use the information as a guide to discuss their treatments with their own physicians. This site does not promote nor endorse the unauthorized practice of medicine by non-physicians or state licensed health care providers.
Medicine is a constantly changing science and not all therapies are clearly established. New research changes drug and treatment therapies daily. The authors, editors, and publisher of these artciles have used their best efforts to provide information that is up-to-date and accurate and is generally accepted within medical standards at the time of publication. However, as medical science is constantly changing and human error is always possible, the authors, editors, and publisher or any other party involved with the publication of this article do not warrant the information in this article is accurate or complete, nor are they responsible for omissions or errors in the article or for the results of using this information. The reader should confirm the information in this article from other sources prior to use. In particular, all drug doses, indications, and contraindications should be confirmed in the package insert.
